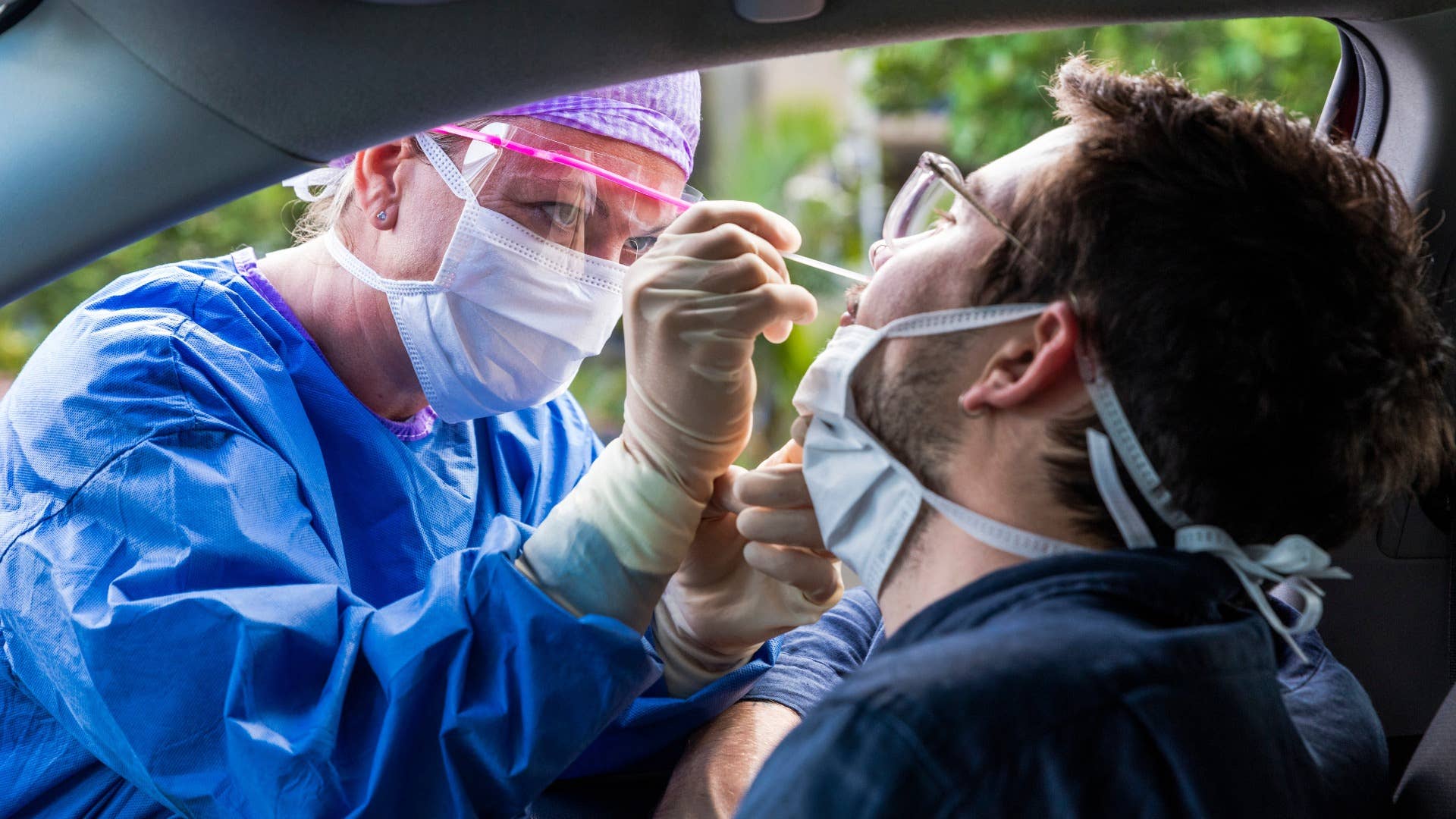
As new confirmed COVID-19 cases rise, hospitals in Utah are preparing to start rationing care.
Per Utah Hospital Association president Greg Bell, who spoke with the Salt Lake Tribune over the weekend, state hospital administrators went to Governor Gary Herbert last week with a list of proposed criteria that should be implemented with regards to who should be allowed to stay in increasingly overcrowded ICUs.
"We're down 20 percent to 30 percent. Hundreds and hundreds of nurses are not able to work as they were [before] because of their own disease or infection in the family, or they're moms and dads with school issues," Bell, who noted that he doesn't currently see any reason why the criteria wouldn't be requested to be activated in a week or two, said. "Some are worn out, some are on leave because they've been doing this for seven months."
The problem is uniquely multi-faceted, with the needs of a pandemic not able to be magically fixed simply with the addition of more ICU beds. In short, upping the number of beds would only have the desired effect if the increase in numbers is able to be met with an appropriate amount of doctors and nurses. Understaffing, meanwhile, has already been an issue.
As for the nature of the proposed criteria brought to Gov. Herbert last week, the report explains that—under Herbert's required approval—it would mean that patients who "are getting worse despite receiving intensive care" would be the first to be moved out. From there, measures would be put in place that—should two patients have equal conditions, for example—would prioritize the younger patient over the older one.
As it stands now, ICUs in Utah have been at an occupation level of around 75 percent, though Bell cautions that such an estimate can be misleading due to the fact that hospitals are already not able to operate at their maximum level.
The total number of COVID-19 cases nationwide is currently nearing 9 million, with nearly 225,000 confirmed deaths.